Osteoarthritis
Proudly serving Tarzana, Agoura Hills and Los Angeles County
What is osteoarthritis?
Also referred to as degenerative joint disease, osteoarthritis (OA) is a chronic disease that can occur in a number of joints, including the hands, shoulders, feet, knees, hips, neck, and lower spine. In normal joints, cartilage covers the ends of the bones, providing a cushion and a smooth gliding surface for joint mobility. In OA, this cushion wears down and begins to cause symptoms such as pain, stiffness, swelling, popping/cracking, and decreased mobility. There are a number of factors that can contribute to osteoarthritis, such as age, previous injury/surgery, excessive weight, genetics, or occupational factors.
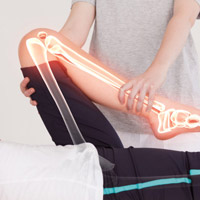 Management
Management
Osteoarthritis is easily diagnosed with radiographs obtained in clinic. There is no cure, but treatments are available to manage symptoms and to slow down the disease process. This includes weight management, activity modification, physical therapy, analgesics and non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroid injections, viscosupplementation, platelet-rich-plasma, and assistive devices.
One of the most beneficial forms of treatment includes physical therapy. Strengthening exercises build muscle around the affected joint, decreasing impact on the joint and reducing pain. Range of motion exercise help maintain and improve joint flexibility and reduce swelling and stiffness. It is encouraged for patients to remain somewhat active, as studies have shown that complete inactivity is contraindicated and can lead to further progression of the arthritis.
Corticosteroids are strong anti-inflammatory medicines that may be used for patients who do not improve with conservative measures. The medication is injected into the joint, under ultrasound guidance, and results in reduced pain and inflammation caused by the underlying arthritis. With this modality, the goal is to alleviate a patient’s pain, allowing them to maximize physical therapy.
Viscosupplementation, also known as hyaluronic acid, is a medical procedure during which a gel-like lubricating fluid is injected into a joint under ultrasound guidance. Hyaluronic acid occurs naturally in joint fluid, acting as a shock absorber and lubricant. However, the acid appears to break down in people with arthritis. Adding hyaluronic acid to the arthritic joint will facilitate movement, reduce pain, and keep the arthritis at bay. Ideally, this procedure should be performed every 6-12 months to prevent the progression of arthritis.
Biological therapies for knee osteoarthritis, such as platelet-rich plasma, are also available and may improve clinical and structural outcomes by delivering a high concentration of growth factors. This therapy may reduce pain, inflammation, and improve overall functionality. Studies have shown PRP may be utilized in the management of tendon and muscle injuries as well as osteoarthritis.